User Story: Lifetime approach in microsimulation modelling to curb the burden of NCDs

Incorporating a lifetime approach in microsimulation modelling to curb the burden of lifestyle-related chronic diseases
Need for early interventions to prevent and control NCDs
Elly Mertens, post-doc research fellow at the Institute of Tropical Medicine (ITM; Unit of Non-Communicable Diseases, Department of Public Health): “The number of people living with and developing non-communicable diseases (NCD), including obesity, diabetes, cardiovascular disease and cancer, has increased rapidly over the past decades. Nevertheless, this public health burden is largely preventable through lifestyle changes. To prevent and control NCDs in future generations of adults, it is key to formulate effective prevention strategies at the right time and to the right populations, allowing efficient use of resources.
Incorporating a life-course approach through microsimulation modelling
Simulation modelling is an essential tool for understanding the influence of lifestyle, including diet, on the progression of NCDs, in particular when a life-course approach is incorporated. Instead of modelling at the population level, in this project, the simulations will be performed at the level of the individual (microsimulation). This is because lifestyle habits and their influence on disease risk tend to vary a lot between individuals within a population. The main challenge in the development of such a life-course NCD microsimulation model is to formulate for each individual its potential health trajectory based on its individual-specific risk profile, and this as accurately as possible using nationally-representative population health data and established resources.
Incorporating variability in individuals’ risk profiles

Lifestyle habits tend to vary to a large degree between individuals within a same population, and therefore also their risk for developing NCDs. For example, person A consumes daily sugar-sweetened beverages (SSBs), while person B does never consume any SSBs, and person C has lowered consumption over the years. In this simplistic example, because of the high SSBs consumption, person A might have higher probabilities for developing NCDs, but does not necessarily develop one, as also depending on other risk factors and a little bit of luck. All of this kind of variability in risk profiles between individuals as well as 'the luck factor’, will be incorporated in the life-course microsimulation modelling. In the current implementation of the model, individual risk profiles account for demographic variables (like age, sex, region and educational level), lifestyle factors (including BMI and waist circumferences) and past history of disease (like high blood pressure, high blood glucose, diabetes, among others).
Microsimulation model focusing on disease burden
Using nationally-representative health data and established resources, as provided by the latest Belgian Health Interview Survey [2018] complemented by the Belgian Health Examination Survey [2018], a synthetic population has been generated in which each individual living in Belgium has its own risk profile. Subsequently, starting annually since 2018, each individual enters our microsimulation model with the aim of forecasting its health trajectories for the coming years. In the current implementation, we aim to estimate the burden of type 2 diabetes [T2D] up to 2030 for each synthetic individual.
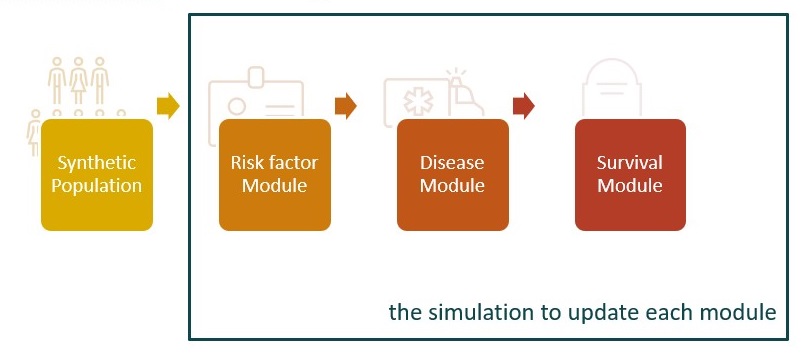
For this, in one-year intervals, each synthetic individual is subjected to the following consecutive modules: 1) Risk factor module, i.e. increase age by one year and update of the risk factors for NCDs using strata-specific [1] transition probabilities of experiencing a change in risk profiles; 2) Disease module, i.e., update of T2D status in T2D-free individuals by recalculating its probabilities of developing T2D; and 3) Survival module, i.e., update of the survival status using probabilities of death, and repeat all this until the individual dies or the simulation period ends. After all individual transitions are combined, the model’s output is an estimate of the burden of T2D in the synthetic population, including all changes in risk factors (in particular overweight/obesity), incident T2D and survival status occurring during the simulation period.
Elly Mertens: “The current implementation of the model aims to forecast the T2D burden up to 2030; this is focused on estimating the number of prevalent and incident cases of diabetes up to 2030. Future implementations will incorporate the influence of diet on the progression of T2D, allowing to estimate the number of preventable cases through diet.
Supercomputing allows to include sizeable information
The larger the population, the more accurately the estimates on disease burden can be calculated. Using the HPC infrastructure of VSC allows to include the sizeable information pertinent to all residents of Belgium, including children and adults as well as newborns, who can be processed simultaneously through the microsimulation model, implying a large number of computationally-intense iterations in parallel.
Scientific impact & benefits
Once the model is operative (developed, finalized and validated), the microsimulation model will quantify the influence of lifestyle on the progression of NCDs in Belgium, particularly the influence of diet. In this regard, the model gives insights into the complex and interlinked causal epidemiological pathways of diet and NCDs from early life to death, including a characterization of diet-related NCD disparities.

The life course NCD microsimulation model will also unravel and identify the population (sub) groups with the highest preventable NCD burden and how early-life dietary habits influence NCD progression throughout life.
Elly Mertens (ITM): “If we consider, for example, schoolchildren who are provided with a piece of fruit once a week at a school day, we could model the schoolchildren for the coming 50 years to see how this fruit provision program would reduce their incidence of overweight/obesity and T2D, and thus estimate how many obesity and T2D cases could be prevented by this health promotion strategy.”
Microsimulation modelling offers opportunities for public health planning
In addition, the successful deployment of this life course NCD microsimulation model would offer great opportunities for public health planning in Belgium.
Elly Mertens: “The methodology developed in this project will provide an improved understanding of the burden of NCDs, including the characterization of its drivers, offering key insights to tailor, prioritize and implement public health strategies in cost-efficient manners.”
By bringing additional inputs to the model (e.g., efficacy of food policies and associated costs), the model can perform comparative-effectiveness of food policies on overall NCD risk and costs.
Elly Mertens (ITM): “Although the ultimate goal of our model is to estimate the diet-related NCD burden for Belgium, the model would also allow exploring the potential impact of food policy measures like, for example, the effect of introducing food pricing strategies like an SSBs tax, food labelling, school-based interventions, amongst others. Given that these food policy measures do change diet, and subsequent NCD risk, this allows for identifying the key food policies for improved population health with sensible use of resources.”
[1] In statistics, a stratum (plural strata) refers to a subset (part) of the population (entire collection of items under consideration) which is being sampled. More info
List of abbreviations
NCDs: Non-Communicable Diseases
SBBs: sugar-sweetened beverages
BMI: Body Mass Index
T2D: type 2 diabetes
Published on 04/03/2023

Elly Mertens (born in 1992) obtained her PhD in Epidemiology from Wageningen University in 2020 and joined ITM the same year. With her strong background in nutritional epidemiology and diet modelling, her main tasks are related to developing a novel life course microsimulation model capable of capturing the contribution of diet to the whole spectrum of NCDs across the lifespan.